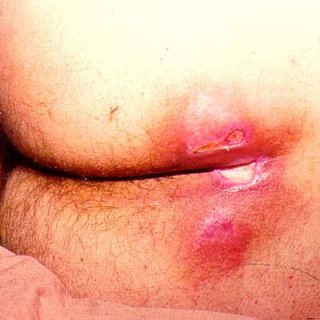
PRP in Burn Ulcers, Bed Sores& Pressure soresand Diabetic Foot Ulcers:
There are studies evaluating the effects of PRP on wound healing. In the early phase of wound healing, the clot formed in the injury area serves as a matrix for cell migration, and this phase is primarily affected by platelets. Platelets contain over 1100 proteins, including growth factors, immune system mediators, enzymes, enzyme inhibitors, and bioactive compounds involved in the wound healing process.
PRP contains important growthfactors deposited in alpha granules of platelets and plasma proteins such as fibrin, fibronectin, and vitronectin. Topical application of PRP accelerates the reepithelialization process by upregulating regulatory proteins of cell cycle such as cyclin A and CDK4. PRP is a potent matrix metalloproteinase (MMP)-1 stimulator and, thus, allows the extracellular matrix to be reorganized during wound healing.
PRP may also suppress inflammation by suppressing cytokine release and increases regeneration and reepithelization by triggering capillary angiogenesis. The involvement of macro- phages in the wound healing process is also mediated by signal proteins released from platelets. PRP has also been reported to exhibit antimicrobial activity against microorganisms such as Escherichia coli, MRSA, Candida albicans, and Cryptococcus neoformans and to have analgesic effect.
Additionally, the pH 6.5–6.7 of the PRP may explain its antibacterial property. Although it has been suggested that leukocytes in PRP accelerate the recovery of soft tissue injury by suppressing bacterial growth, it has been also claimed that PRP may cause local pain and even suppress the healing process due to the inflammatory cytokines in it.